WASHINGTON — Surrounded by hot pink lights and cherry blossom pink drapes on a ballroom stage, family doctor Marguerite Duane offered a seemingly simple solution to infertility: Doctors should have conversations with young girls about whether they want to have children one day.
“I have these conversations with children starting at 8, 10, 12 years old: What do you want to be when you grow up?” Duane said. If you’re a child who wants to be a doctor, for instance, “there are things you need to put in place. If you hope to have children one day, there are things that you need to consider and have the conversation early.”
The proposal from Duane, a specialist in restorative reproductive medicine who is affiliated with the anti-abortion Charlotte Lozier Institute, got a warm reception from the audience gathered for the Trump administration’s inaugural National Conference on Women’s Health.
The three-day event hosted by the Department of Health and Human Services last week was designed to “explore breakthroughs in research, prevention, diagnosis, and treatment of health conditions that affect women across the lifespan.” Government officials hosted an eclectic mix of wealthy philanthropists, alternative medicine influencers, health tech executives, and medical researchers to discuss a wide range of issues, from Lyme disease to gut health.
Seeking to reach women at a moment when President Donald Trump’s support is slipping among a key voting bloc, the Make America Healthy Again movement, the administration-sponsored event elevated perspectives outside conventional standards of medical care and counter to many women’s health choices.
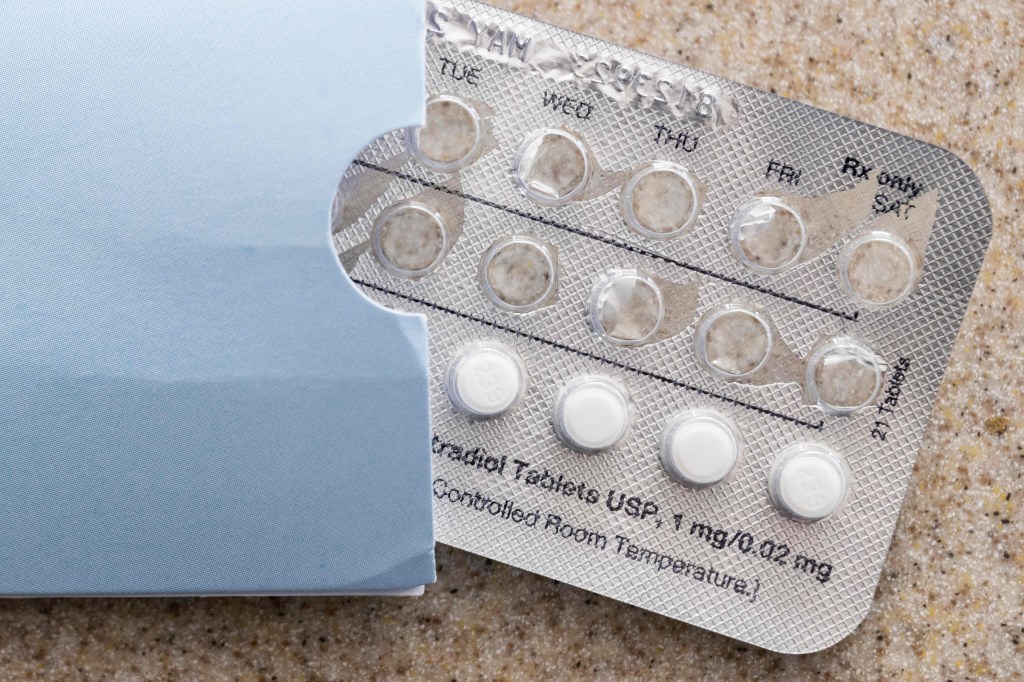
For example, during a 40-minute panel hosted by Alexis Joel, the wife of musician Billy Joel, several doctors raised concerns about how frequently hormonal birth control is used to treat women’s health symptoms. Duane and the two other female physicians on the panel said they were uncomfortable with the idea of using birth control pills for their own treatment, noting that their “values” or “cultural perspective” did not align with use of the medication.
Nearly a third of U.S. women ages 18 to 49 report having used birth control pills in the previous 12 months, according to a 2024 KFF survey. In addition to their use as a contraceptive, the pills are prescribed for a variety of health issues, including preventing anemia from heavy periods and treating uterine fibroids.
Joel, who has spoken publicly about her experience with endometriosis, brought her own doctor, Tamer Seckin, to discuss the common, painful condition, in which thick tissue develops outside of the uterus. Seckin said women’s concerns about menstrual pain are often dismissed by doctors, leading to missed diagnoses.
Asima Ahmad, a doctor who specializes in fertility and co-founded Carrot, a company that offers job-based fertility benefits, offered another explanation for why the disease is overlooked.
“As providers, we should learn how to treat it, rather than covering it up with birth control pills or progesterone,” she said.
Hormonal birth control pills, which help slow the growth of new tissue, are one option for treating endometriosis, according to the American College of Obstetricians and Gynecologists.
Andrea Salcedo, a California OB-GYN on the panel who said she has endometriosis as well, said she declined birth control as a treatment. She noted her decision aligned with her “values,” in particular her desire to have more children.
“Is this all that we can do?” Salcedo said of being offered birth control.
Salcedo said she prescribes alternative treatments to her patients because she believes the root cause of infertility is directly related to gut health. Cod liver oil and vitamin A top her list, she said.
It is unclear whether there is an association between vitamin deficiencies and endometriosis. Taking too much vitamin A can cause health problems, including birth defects if taken while pregnant.
Those supplements have been touted by HHS Secretary Robert F. Kennedy Jr. — including, falsely, as a treatment for measles during an outbreak in Texas last year.
About a quarter of U.S. adults wrongly believe vitamin A can prevent measles infections, according to a KFF poll conducted last year.
The panel also coalesced around the idea that a lack of knowledge is the root problem: Girls do not receive enough education on how to become pregnant or identify the warning signs of infertility, the doctors suggested.
Education has become too hyperfocused on preventing pregnancy, Ahmad said.
“I was in junior high, and I was learning about trying not to get pregnant, and I was scared that if I sit in a room with a guy alone, I will,” she said. “They put all of this fear into it, but family planning isn’t just about preventing pregnancy. It’s about learning about how to build your family.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism. Learn more about KFF.
USE OUR CONTENT
This story can be republished for free (details).